 |
|
ENT Examination Unit |
Otolaryngology or ENT |
|
ENT Treatment Unit,
Medical Unit |
ENT Examination
Technique |
|
Malignant tumors of an
ENT organs |
ENT Treatment Unit
Summary |
|
| �� |
|
ENT Examination Unit |
Only 2 compressors for both positive pressure
and negative pressure with little noise and
vibration;
Available to operate it simultaneously on both
sides;
Advanced spray rod for the pulverization of liquid
medicine;
Discharge pollution automatically;
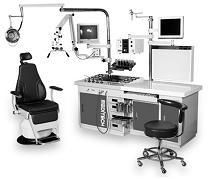
Stable performance in heating;
Technical parameter
Positive pressure pump: 2. 5kg / cm2; negative
pressure pump: 740mm Hg; main suction bottle:
3000CC; sub suction bottle: 1000cc; cleaning device:
air filter regulator;
Power: 1000w; voltage: 220v; frequency: 50 / 60HZ;
throat preheater: 250w; weight: 15kg; cold light
source: 250w; dimension: 145 (w) *73 (D) *90 (H) ;
Standard layout
Spray rod: curved 2pcs, straight 4pcs; suction
device: 2pcs; blow device: 2pcs; spot light: 2pcs,
100-150w; tray: 1pc, 36*27cm; tampon container:
2pcs.
Optional accessories
Endoscope; endoscope optical impression system;
image management system; ENT operating chair; cold
light source |
| Article Source: |
| http://www.hiwtc.com/products/ent-examination-unit-2836-9294.htm |
|
Back To Top |
| �� |
|
ENT Treatment Unit,
Medical Unit |
Description features:1)
As medical equipment that this device is used when
doctor treats patient at E.N.T hospital.
This unit is medical treatment device for E.N.T
which is consisted of spray for medical treatment,
suction, illumination, instrument tray, instrument
can and antifog device.When this equipment operates
because of anti_noise heating device, noise does not
produce and it is stoped automatically, after
heating.This device is installed ultraviolet
sterilizer, so can sterilize scope, instruments in
253.7nm��5% wavelength.As using japanese spray of
good quality, breakdown is low.Instruments tray is
maintained warm, because instruments tray is kept at
fixed temperature(40��C), so patients received
treatment with warm instruments (OPTION)By using
Power LED in Penlight, doctor can observe precisely
through light.This unit is installed "ENDOSCOPE
infrared sterilizer", is hygienic and there is
effect of Anti-fog and Endoscope storage is
convenient.(OPTION)Specifications of ENT Treatment
Total Unit cham CU-3000
Power SourceAC 220V, 50/60Hz
Power Consumption1200VA
Suction Motor(Main suction) 250W, GAST Oilless Motor
pump
Max. Negative pressure 680mmHg,
Exhaust Volume 133.3 liter/min.
(Sub suction) 250W, GM TECH Oilless Motor pump
Max. Negative pressure 680mmHg,
Exhaust Volume 90 liter/min.
Dimension1800(W) x 709(D) x 850(H), POSTPOLE :
1925(H)mm
Net WeightApprox.127kg
Air CompressorPressure 1.0kgf/cm2 ��0.3Kg/cm2
Ultraviolet Sterilize 253.7nm �� 5%
Standard
Accessorieslllumination cool-ray lamp (220V, 100W)
Medicine bottle : White / Brown / Blue
Ointment Jar
Spray(Straight / curved)
Nasal Suction tip (#1~4)
Nasal Ventilation tip (#1~4)
Waste receptacle 105mm
Main suction bottle (3000cc)
Sub-suction bottle (1000cc)
Instrument tray with cover
Gauze container with cover
80mm can
53mm can
Chair connect consent (10P)
Warmer switch
Used Instrument receptacle
Endoscope UV sterilizer set
Main Fuse(10A)
Main Suction Fuse(4A)
Sub suction Fuse(3A)
Comp Fuse(4A)
Optional
AccessoriesMicroscope with Light source & Arm set
Post pole #2
Film View box with arm set
14" Monitor & Arm base set
CCD Camera mounted on the base set
Telescope Hander Related Keywords: Surgical Tables,
Medical FurnitureView More details for this product
|
| Article Source: |
| http://www.himfr.com/d-p115449544470257900-ENT_Treatment_Unit_Medical_Unit/ |
|
Back To Top |
| �� |
|
ENT Treatment Unit
Summary |
We ply a broad gamut of
ENT Treatment Unit and
ENT treatment unit which is highly characterized with its functions. ENT Examination Unit is exemplary
sized model which is widely used in E.N.T. E.N.T
treatment Unit in which the required tools for
spray, vent &anti-fog function to be used for the
medical examination & treatment of ear, nose and
throat are installed. It is installed with Anti-fog
system. It can be used with ENT chair and visual
system. ENT Examination Unit can be operated and controlled by the
switch in the control panel providing the easy and
comfort treatment. The high tech design gives
easy-installation and maintenance, flexibility of
space and convenient patients-treatment. E.N.T chair
operated full- automatically for the function of
position setting (up, down, lie, rise, and rotation)
according to the purpose of ear, nose and throat
treatment or operation. It is fully automatic oil
pressure examination chair which is generally used
in E.N.T and Medicine part.
characterized with its functions. ENT Examination Unit is exemplary
sized model which is widely used in E.N.T. E.N.T
treatment Unit in which the required tools for
spray, vent &anti-fog function to be used for the
medical examination & treatment of ear, nose and
throat are installed. It is installed with Anti-fog
system. It can be used with ENT chair and visual
system. ENT Examination Unit can be operated and controlled by the
switch in the control panel providing the easy and
comfort treatment. The high tech design gives
easy-installation and maintenance, flexibility of
space and convenient patients-treatment. E.N.T chair
operated full- automatically for the function of
position setting (up, down, lie, rise, and rotation)
according to the purpose of ear, nose and throat
treatment or operation. It is fully automatic oil
pressure examination chair which is generally used
in E.N.T and Medicine part. |
| Article Source: |
| http://www.megamedicals.com/ent-treatment-unit.htm |
|
Back To Top |
| �� |
|
Malignant tumors of an
ENT organs |
From all cancerous neoplasms on a lobe of an ENT
of organs 23 %, at men - 40 % are necessary, and the
larynx cancer prevails. 65 % of all tumours of an
ENT of organs are taped in the started condition. 40
% of patients die, not having lived and 1 year from
the moment of diagnosis statement.
At sick the diagnosis at 34 %, a pharynx cancer - 55
% was a larynx cancer erroneous. At patients with
localisation of tumours in a nasal cavity and its
adnexal sinuses the erroneous diagnosis compounds 74
% of cases.
Thus it is possible to draw a conclusion, oncologic
vigilance, especially in an
ENT Examination
Unit should be how much
great.
Proceeding from classification of 1978 excrete:
>Not
epithelial tumours:
>Soft
tissues (connective-woven)
>The
neurogenic
>Tumours
from a muscular tissue
>Tumours
from a fatty tissue
>Neuroepithelial
tumours of bones and cartilage
>Epithelial
>Tumours
of a lymphoid and hemopoietic tissue
>Enclavomas
>Secondary
tumours
>Tumour-like
formations
>In
each of the given bunches excrete benign and
malignant tumours. Also apply classification by
system TNM.
��1 - The tumour occupies one anatomical part.
��2 - The tumour occupies 2 anatomical parts, or 1
anatomical part, but sprouts the next organ, amazing
no more than one anatomical part.
��3 - The tumour occupies more than 2 anatomical
parts, or 2 anatomical parts + germination in next
organs.
N0 - There are no regional metastasises
N1 - Regional metastasises secund and displaced
N2 - Regional metastasises bilateral displaced
N3 - Regional metastasises secund nonmotile
N4 - Regional metastasises bilateral nonmotile, or
the secund conglomerate of metastasises sprouting in
the next organs
��0 - There are no remote metastasises
M - is the remote metastasises
Larynx malignant tumours
The cancer, almost always planocellular prevails, is
rarer basal cell cancer. The larynx sarcoma meets
was rarely.
The larynx cancer occupies 4 place among all
malignant tumours from men, concedes to a carcinoma
of the stomach, lungs and an esophagus. A case rate
interrelation, a carcinoma of a larynx at men and
women 22:1.
There is a cancer of a larynx at persons more
youngly 30 years and is more senior 40 years, and at
women 20 years are younger.
To brake the top part of a larynx - average is
amazed, is even rarer - the inferior part.
Mainly there is an exophytic form of a cancer which
grows slowly. At a tumour of an epiglottis process
extends upwards and to front, at have swelled up
average part of a larynx through a commissure or a
guttural ventricle diffusion goes on the top part.
The tumour of the inferior part of a larynx grows
downwards through pencil-point ligament inpours on
forward parts of a neck.
Earlier metastasizes a cancer of a vestibule of the
larynx more often on the lesion party, and most
slowly at a tumour of forward part of a larynx.
Excrete 3 seasons of development of tumours of a
larynx:
>Initial
- tickles, inconvenience at swallowing, sensation of
a lump in a throat
>The
season of full development of disease - arises
hoarseness up to an aphonia, difficulty of breath up
to an asphyxia, disturbance of swallowing up to full
impossibility
The innidiation season
>The
differential diagnosis spend with a tuberculosis, a
scleroma, a syphilis. (Solving) histological
research or carrying out of preventive therapy
without enough good result is definitive.
ENT Examination Unit. More often - the
larynx extirpation, is rarer - its resection, is
even rarer - reconstructive operations. Before to
start to surgical to treatment, necessarily effect a
tracheotomy, for carrying out of an incubation
narcosis, and for breath maintenance in the
subsequent postoperative season.
Kinds of operations at a larynx cancer:
Endolaryngeal the oncotomy - is shown at a tumour of
1 stage, average part
Oncotomy outside access: and. A thyrotomy, a
laryngofissure - at 2 stages, an average floor;.
pharyngotomy infrahyoid. Effect at tumours of an
unstable part of an epiglottis an epiglottis
extirpation.
Larynx resection. Effect at tumour localisation in
lobbies of 2/3 vocal cords with diffusion on a
precomissure; at a lesion of one vocal cord; at the
circumscribed cancer of the inferior part of a
larynx; at the circumscribed cancer of the top part
of a larynx under a condition inaction arytenoid
cartilages.
Kinds of resections:
Lateral (sagittal)
Frontlateral (diagonal)
Lobby (face-to-face)
The horizontal
The laryngectomy - is effected, if the resection is
impossible, or at the third stage
The amplate laryngectomy - leaves a larynx, a
sublingual bone, a tongue root, lateral sides of a
laryngopharynx. Operation invalidating. As a result
the tracheostomy is formed and the esophageal probe
for a food is introduced
Except surgical, use radial treatment. It start to
perform before operation in 1 and 2 stages of
process. If after half of sessions of treatment
appreciable retrogress of a tumour radial therapy
continue to a full dose (60-70 Gray) becomes
perceptible. In cases when after half irradiatings
retrogress of a tumour less than 50 % radial therapy
interrupt and operate the patient. The cancer of an
average floor of a larynx, and a cancer of the
inferior part radio resistant is most
radiosensitive. In case of presence of regional
metastasises effect Krail's operation - the fat of
lateral part of a neck, deep bulbar lymphonoduses,
noddle muscles, an intrinsic bulbar vein,
submandibular lymphonoduses, a submandibular
sialaden leaves. In case of presence of the remote
metastasises it is spent symptomatic and
chemotherapy. An exception are metastasises in
lungs, their operative treatment here is admissible. |
| Article Source: |
| http://knowledge-storage.com/medicine/37-medicine/155-malignant-tumors-ent-organs |
|
Back To Top |
| �� |
|
Otolaryngology or ENT
|
Otolaryngology
Otolaryngology or ENT (ear, nose and throat,ENT Examination Unit)
is the branch of medicine that specializes
in the diagnosis and treatment of ear, nose, throat,
and head and neck disorders. The full name of the
specialty is otolaryngology-head and neck surgery.
Practitioners are called otolaryngologists-head and
neck surgeons, or sometimes otorhinolaryngologists (ORL).
Otolaryngology is one of the most competitive
specialties to enter for physicians.
The term comes from the Classical Greek roots ὠ��- -
ot- (root of ��ὖς) "ear", �˦��ѦԦæ�- - laryng- (root of
��ά�ѦԦæ�) "larynx/throat", and the suffix -logy
"study", and it literally means "the study of ear
and neck".
The full term otorhinolaryngology (Neoclassical
Greek and Modern Greek: ὠ�Ӧ�(��)�ѦɦͦϦ˦��ѦԦææϦ˦Ϧ�ί��),
also includes ῥ�ɦͦ�- - rhino- (root of ῥίς) "nose".
Explanation
Otolaryngologists are medical doctors (MD, DO, MBBS,
MBChB, etc.) who, in the United States, complete at
least five years of surgical residency training.
This is composed of one year in general surgical
training and four years in otolaryngology - head and
neck surgery; in the past it varied between two and
three years of each.
Following residency training some otolaryngologists
elect to complete advanced subspeciality fellowship
training which can be 1�C2 years in duration
(pediatric otolaryngology), Neuro-otology, Facial
Plastic and Reconstructive Surgery, Rhinology or
head and neck oncology. |
| Article Source: |
| http://en.wikipedia.org/wiki/Otolaryngology |
|
Back To Top |
| �� |
|
ENT Examination
Technique (ENT Examination Unit) |
Ear Examination
NB. As well as assessing the appearance of the ear,
a complete examination of the ear also involves an
assessment of hearing. This is done in greater
detail in the audiology section but basic tests of
hearing can be done in the clinic or bedside.
History
The classic symptoms of ear disease are:
��deafness
��tinnitus
��discharge
(otorrhoea)
��pain (otlagia)
��vertigo
as well as these you may need to ask about other
relevant features in the history:
��previous
ear surgery
��head
injury
��systemic
disease (e.g storke, multiple sclerosis,
cardiovascular disease)
��otoxic
drugs (antibiotics, diuretics, cytotoxics)
��exposure
to noise at work or recreation (shooting)
��family
history of deafness
��history
of atopy and allergy in children
Inspection
Before examination with the otoscope / auroscope,
the external ear should be inspected for any obvious
abnormality including the following:
��Size and
shape of the pinna
��Extra
cartilage tags / pre-auricular sinuses or pits
��Evidence
of trauma to the pinna
��Suspicious
skin lesions on the pinna including neoplasia
��Skin
conditions of the pinna and external canal
��Obvious
infection of the external ear and canal with frank
discharge
Evidence of previous surgery (scars)
The ear canal and drum itself are best examined with
a modern electric otoscope / auroscope. It is
essential that the batteries are in good condition
as a dim light makes examination very difficult.
The pinna should be grasped between fore-finger and
thumb and pulled posteriorly and superiorly during
examination.This has the effect of staightening out
the canal which normally has a slight curve, and
allows better inspection of the tympanic membrane
(TM) or eardrum. Very small infants and neonates
have slightly different anatomy and it is usally
recommended that the pinna is pulled posteriorly but
not superioirly for examiation.
An appropriate sized end should be fitted on the
otoscope.Although it is tempting to use a small end
to make insertion easier, this severley restricts
the image available, and the best view is acheived
by using the largest end that will fit into the ear
canal.
Holding the otoscope near the eyepeice end makes it
less likely that you will cause the patient
discomfort by making sudden or exagerated movement.
Holding the otoscope by it's end can lead to
increased discomfort because movement of the hand is
exaggerated in the ear
As well as the TM itself, make note of the condition
of the the canal skin, the presence of any wax and
any foreign body or discharge.
Tympanic Membrane
Although textbooks usually contain excellent
pictures of the whole tympanic membrane, these are
usually taken with wide angled endoscopes and using
the otoscope, it is not always possible to see the
whole drum in one single view. This is particulalry
true where the anterioir wall is very prominent, and
you will have to move the otoscope about to see the
whole drum in several different views.
The drum is roughly circular and around 1cm in
diameter. In a normal drum you should be able to
identlify the following:
��Handle /
lateral process of the malleus
��Light
reflex / cone of light
��Pars
tensa and pars flaccida (attic)
ENT Examination Unit is occasionally possible to see some of the
following structures through a very healthy thin
drum:
��Long
process of incus
��chorda
tympani
��eustachian
opening
��promontory
of the cochlea
You should be able to identify some of the commoner
pathological conditions related to the eardum:
��perforations
��tympanosclerosis
��Glue ear
/ middle ear effusion.
Retractions of the drum
Haemotympanum (blood in the middle ear)
The mobility of the eardrum can be assessed by using
a pneumatic speculum which attaches to the otoscope.
This takes a bit of manual dexterity and practice,
and is done more objectively using a tympanometer.
(see audiology section)
If you are suspicious of any serious ear pathology,
check the facial nerve function
Basic tests of hearing
Tuning fork tests.
These test hearing in both ears and can help
distinguish between a sensorinueral and conductive
hearing loss (for more details see section on types
of deafness)
Ideally you should use a 512Hz tuning fork. If
unavailable a 265Hz will suffice. Strike the tuning
fork against your elbow or knee to make it vibrate.
(this takes practice and may hurt if you get carried
away...)
Striking it against a metal object can introduce
unwanted harmonic vibrations into the sound signal.
DO NOT hit the patient on the head with it.
Tell the patient what you are doing and what you
want them to do before you put the fok against their
head. If you talk to them while you are doing the
test it may confuse the result.
Weber Test Place the fork in the middle of the head
(vertex). Ask the patient if he can hear the sound
equally in both ears, or if it is louder on one
side.
If the patient cannot hear the sound at all, try
striking the fork again, or pressing it against the
nose
......or even the upper teeth in the midline as this
facilitates bone conduction
A patient with normal hearing should hear the sound
equally in both ears.
If a patient has a unilateral conductive loss, the
Weber will localise to the affected ear. (try
putting your finger in your ear to block it up and
repeat the test). If a patient has a unilateral
sensorineural loss, the Weber will localise to the
opposite / unnafected ear.
Rinne Test Place the fork behind the ear, pressing
on the mastoid process (firmly)
and then hold the fork about three inches away from
the ear .
In a normal ear, the patient should hear the tuning
fork louder in front (air conduction) and quieter
behind (bone conduction). This is called a Positive
Rinne test. If the patient has a conductive hearing
loss (usually of around 20dB or greater) then they
will hear the bone conduction (behind the ear)
louder than the iar condution and this is called a
Negative Rinne test.
If a patient has a non-hearing ear on one side
('dead' ear), then they will still hear the bone
conduction louder, becuase the sound will be
transmitted around the skull and heard by the other
cochlea. This is called a False Negative Rinne test.
Interpertation of Weber and Rinne Testing
Basic tests of hearing.
To make a basic assessment of a patients hearing,
you need to mask the non test ear, say by inserting
your finger into it, and then ask them to repeat
random numbers (e.g 31, 45, 17, 64 etc) that you
speak into the test ear. Start with a quiet whisper,
then a 'stage' whisper, then quiet speech, loud
speech and finally a shout, stop at the level at
which the patient can accurately repeat the numbers
you are giving them.
ENT Examination Unit is important that they cannot see your face as
many deaf patients can lip read. Repeat this on the
other side and you can get a rough measure of their
hearing.
You could report this as (for example) "able to hear
a quiet whisper at arms length on the right ear, but
only able to hear a loud converationsal voice at
arms length on the left"
Very roughly this might equate to the following
level of hearing loss:
Able to understand following speech level at arms
legth Hearing loss equivalent
Quiet whisper Normal
Loud whisper 20-30dB
Quiet voice 30-45dB
Loud voice 45-60dB
Shout 60-80dB
Hearing levels are objectively and accurately
assessed by pure tone audiometery. (see Audiology
section)
Ear Nose Throat Neck
Examination of the Nose
Examination of the nose also involves assessment of
function: airway resistance and occasionally sense
of smell. Examination of the nose is incomplete
without looking into the mouth and pharynx.
History
The main symptoms of nasal disease are:
��airway
obstruction
��runny
nose (rhinorrhoea)
��sneezing
��loss of
smell (anosmia)
��facial
pain due to sinusitis
��snoring
associated with nasal obstruction
In addition you may like to ask questions about some
of the following, where relevant:
��Allergies
/ atopic disease
��Smoking
��Pets at
home
��Occupation
History of previous surgery
History of trauma
General medical history
Seasonal or daily variation in symptoms
Inspection
Look at the external nose and face before you look
into it. Ask the patient to take off any glasses
they may be wearing. Look at the nose from the side
as well as in front. A deviated nose is often best
looked at by looking from above. Look for any of the
following:
��Obviously
bend, deformity or swelling
��Scars or
abnormal creases across the nose
��Redness
or evidence of skin disease
��Discharge
or crusting
��Offensive
smell
To inspect the nose, fist look into the very front
of the nose (anterior nares) by tipping the tip of
the nose up with a finger and looking inside without
a speculum.
After this you may choose to use a speculum with a
torch or head mirror.
Probably the best way of examining the nose for
undergraduates and general pratitioners is to use an
otoscope with a very wide end on it. The head mirror
is excellent for this purpose, but it take a while
to get used to and if you only have two weeks, it
may not be worth your while. Otolaryngologists use
either a head mirror or illuminated spectacles.
The Thudicum speculum is used to open up the nose,
this take practice to use correctly but is very
useful if you wish to instument the nose for any
reason. You will need to be shown how to hold this
correctly.
Inside the nose you should be able to identify the
nasal septum medially and the turbinates laterally.
It should nearly always be possible to see the
inferior turbinate, the middle turbinate may be more
difficult. The superior turbinate is of little
importance in examination and is very small.
Try to assess if there is any inflammation
(rhinitis) and if the septum is straight or deviated
to one side.
If you see what you think is a polyp, it is useful
to see if it is sensitive. Swollen turbinates are
often mistaken for polyps: a polyp is insensitive
whereas a turbinate is quite tender to touch. Try
touching it gently with a blunt probe to measure
this. Polyps tend to have a slightly grey / yellow
colour whereas turbinates or more commonly pink.
In children, a foreign body may occasionally be seen
inside the nose, this is usually accompanied by an
offensive, unilateral nasal discharge.
Look inside the mouth as well, occasionaly large
nasal polyps and tumours may be visible arising from
behind the soft palate. It is not normally possible
to view the nasopharynx on routine examination, and
this is either done using a mirror and headlight or
an endoscope. Undergraduates will not be expected do
be able to undertake this examination.
To assess the nasal airway there are a variety of
bedside techniques: 1. Hold a cold metal tongue
depressor under the nose while the patient exhales.
If there is reasonable airflow, there should be some
condensation under both nostrils.
2. Occlude one nostril with a thumb and ask the
patient to sniff. This gives a reasonable idea of
the patency of the airway.
Of course, the nasal airway changes with posture,
time of day and a variety of other factors, so it is
very difficult to measure the nasal resistance
accurately in a way which reflects the patients'
actual perception of nasal obstruction. A variety of
instruments are in use to attempt to do this (rhinomanometery)
but their use is largely as a research tool.
The smell is not routinely assessed in nasal
examination as this can be very subjective. On
occasions where there is a need to assess smell,
this is done using a series of bottles containing
specific odours. Usually asking specifically about
sense of smell in the history is enough.
Nasal Obstruction and Rhinitis section Facial Pain
and Sinusitis section
Ear Nose Throat Neck
Throat Examination
The throat examination includes a thorough
examination of the oral cavity.
History
As the mouth and throat can have a variety of
different clinical problems it is more difficult to
generalise about history taking.
ENT Examination Unit is always important to ask about a history of
tobacco or alchohol usage and if the mouth is
involved, if there is any relevant dental history. A
number of systemic diseases may present with oral
syptoms and signs - a reasonable medical history is
often required.
Examination
Pressing the tongue down with a wooden spatula and
peering in with a dim torch is often the extent of
the majority of medical examinations of the mouth,
it is however, insufficient. The mouth contains a
number of recesses and sites which are not routinely
examined such as the floor of the mouth, and these
may contain occult malignancies or other pathology.
The mouth should be examined systematically.
Use the brightest torch you can. Start by examining
the mouth without a tongue depressor and note the
condition of the tongue. Pressing down on the tongue
with a tongue depressor wil allow you to examine the
back of the tongue and tonsils (see diagram). You
should also be able to inspect the uvula and soft
palate.
To inspect the hard palate ask the patient to tip
their head back, until you can see the whole hard
palate all the way to the front teeth.
Next examine the buccal region and the gingivolabial
/ gingivobuccal sulcus - the space between the cheek
and the gums, all the way from the front to the back
where the cheek meets the ascending ramus of the
mandible at the so called retro-molar trigone.
Ask the patient to stick their tongue upwards and
now examine the floor of the mouth.
Examination of the nasopharynx and larynx are done
by using mirrors or flexible fibre-optic
nasendoscopes. You will not be required to do this
as undergraduate.
remember that to adequaltely examine the mouth you
should inspect:
��tongue
��hard and
soft palate
��tonsillar
fossa
��gingivolabial
/ gingivobuccal sulci
��floor of
mouth / undersurface of tongue |
| Article Source: |
| http://www.bris.ac.uk/Depts/ENT/otolaryngology%20examination%20technique.htm |
|
Back To Top |
|
|
�� |
|
|
|
| |
|
